CU Gastroenterology Professor Overseeing Trial of Swallowable Gastric Balloon for Weight Loss
11/01/2023
A new device for weight loss — a swallowable gastric balloon that requires no invasive procedures — may soon be approved by the U.S. Food and Drug Administration (FDA) after a nationwide clinical trial that is being overseen by Shelby Sullivan, MD, professor of gastroenterology at the University of Colorado School of Medicine and director of the Metabolic and Bariatric Program.
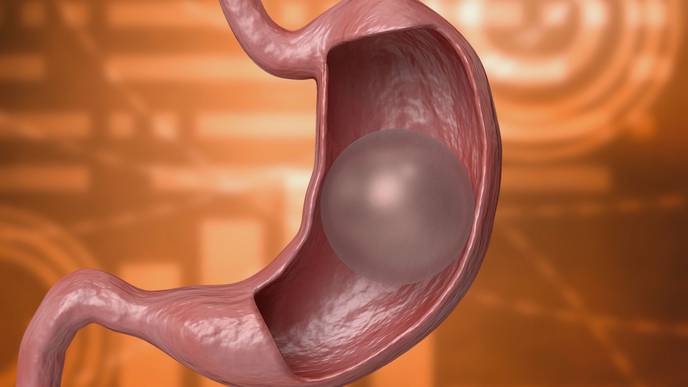
“The balloon is contained in a capsule, and it’s swallowed,” Sullivan says. “It’s attached to a catheter, and once it hits the stomach, we fill it with saline, then we pull the catheter back out through the esophagus. The balloon degrades over the course of four months, then the stomach shoots it out into the small bowel, and it passes out through your stool. There’s no anesthesia; you don't have to come back in. You swallow it, you walk out, and you go home and go on with your daily life.”
Once it’s placed, the fluid-filled balloon helps its recipient lose weight by taking up space in the stomach and reducing gastric motility — slowing the stomach from emptying— making people feel full longer on smaller amounts of food.
Looking at time limits and repeated use
Sullivan was involved in an earlier trial of the gastric balloon, which is manufactured by Allurion Technologies, but the new trial — dubbed the AUDACITY trial — was created to comply with new FDA guidance on short-term devices.
“The FDA has mandated that any short-term device needs to last for at least six months, and this balloon self-deflates at four months,” she says. “This randomized controlled trial gives the balloon patients two balloons. Eight weeks after the first balloon deflates and passes, we place another balloon. The FDA accepts that as six months of balloon dwell time in a one-year period.”
The AUDACITY trial, which Sullivan is leading at 17 sites, with 550 patients, is also looking to see if the gastric balloon is safe for repeated use.
“When you take a weight-loss medication and you stop that weight-loss medication, you start regaining weight right away,” she says. “With balloons, it's different. The weight loss maintenance is pretty good for the first six months after the balloons come out, and even two years later, at least 50% of patients are maintaining their weight. But we recognize that obesity is a chronic disease, and weight eventually comes back on. We need to think about balloons as repeatable therapy.”
Reversible therapy for those with lower BMI
Balloon therapy also is completely and easily reversible, Sullivan says, unlike procedures such as a sleeve gastrectomy, where part of the stomach is removed entirely, or a gastric bypass, which makes changes to the stomach and small intestine that are difficult to reverse.
On the flip side, balloon therapy typically results in 10% to 15% total body weight loss, while gastric bypass can help achieve a 30% overall weight loss. Patients in the AUDACITY trial have a body mass index of 30 to 40.
“We have done meta-analyses that looked at the BMI spectrum, and in general, the studies that have looked at patients with higher BMI outside of the U.S. have seen no difference in total body weight loss in patients with a BMI of 30 to 40 versus those with a higher BMI,” Sullivan says. “But the FDA label indications will be for a BMI of 30 to 40. Any use outside of that would be considered off-label use for patients who are OK with the amount of weight loss that you get with a balloon.”
Managing obesity
As a gastroenterologist who has been involved in endoscopic bariatric studies as well as trials of weight loss medications, Sullivan works with people who are struggling with obesity. And while in general, people know what a healthy diet looks like, she says, it’s difficult to maintain in a culture and environment that seem geared toward promoting obesity.
“Some people are genetically susceptible to obesity,” she says, “and then we're living in an environment where we don't have nearly as much activity in our jobs as we did 60 or 70 years ago, we have easier access to food, and that food is more highly processed, we have more controlled temperature, we have jobs where we're working late at night or overnight, which can affect weight, and on top of all of that, we have chemicals circulating in the environment that are endocrine disruptors and obesogenic factors that promote weight gain.”
Sullivan says in her clinic, she works to take away the stigma and shame that surround obesity to help patients reach their weight loss goals. Whether it’s endoscopic procedures like a balloon, weight-loss medications, or lifestyle modifications — or a combination of all three — there are therapies that work, she says.
“We have rapid advancement in what we're able to do for patients endoscopically,” she says. “Doing combination therapy with endoscopic therapies and weight loss medications is increasing our ability to achieve weight loss that's close to surgical levels.”

Facebook Comments